Your basket
Your basket is currently empty.
Tampon Case for 4 tampons
-£1
ProViotic - 30 tablets
-£1




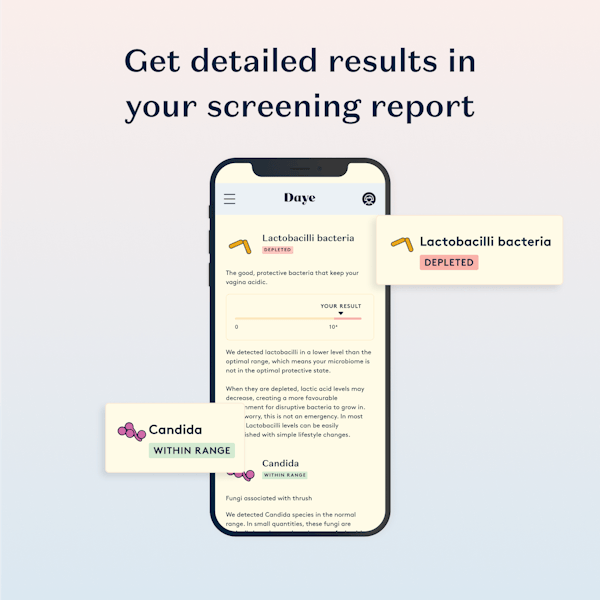
Vaginal Microbiome Screen
Understand your risk of vaginal infections like thrush or BV, STIs, fertility implications, and other gynae health complications using a non-invasive at-home tampon screen.
Taking control of your sexual health has never been easier with Daye's innovative Diagnostic Tampon. All you have to do is insert the tampon, wear it for 20 minutes, and remove. You don’t need to be on your period, which means you can be menopausal, pregnant or on long-term contraception. Ship your return box, and our accredited labs will process your sample.
We use sophisticated molecular PCR - the most accurate method available for detecting STIs and other vaginal infections. Your in-depth results will be available online in just 5-10 days. In addition to your screening report, you'll get access to virtual consultations with sexual health experts, discreet prescription treatment options, and personalised lifestyle recommendations, tailored to your needs.
Once your Daye Diagnostic Tampon sample arrives at our state-of-the-art laboratory, our team of experts will process it. You can expect your personalised results report to be available online within just 5-10 days. We'll send you an email notification as soon as your results are ready to view securely in your private Daye account dashboard. With Daye, you can trust that your vaginal screening results will be delivered quickly, accurately, and discreetly.
Taken from the comfort of your safe space, and used just like a normal tampon, our Vaginal Microbiome screen collects more vaginal fluid than a standard swab and covers the whole vaginal canal. This means it gets the most comprehensive results possible for common infections – plus the ones you might not know.
Frequently bought together
Who is this service for?
If you have recurrent infections
If you have recurrent infections
Our Diagnostic Tampon can check for infection-causing microbes and fungi, as well as your levels of protective, good bacteria.
We suggest screening 2-4 times per year or when symptoms appearIf you have fertility concerns
If you have fertility concerns
The vaginal microbiome plays a vital role in reproductive health, and disruptions can impact fertility.
We suggest a one-off screen to identify all treatable issueIf you are in (peri)menopause
If you are in (peri)menopause
The vaginal microbiome changes during perimenopause, increasing the risk of infections and vaginal dryness.
We suggest two screens per year to maintain a healthy and well-balanced vaginal environmentGet personalised insights into your hormonal balance
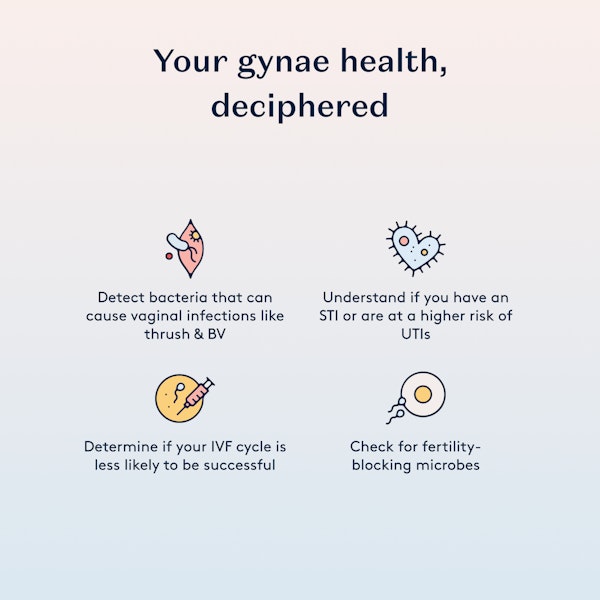
Detect bacteria that can cause vaginal infections like thrush & BV
Understand if you have an STI or are at a higher risk of UTIs
Determine if your IVF cycle is less likely to be successful
Check for fertility-blocking microbes
Choose a screen that works for you
Microbiome + STI + HPV Screen
£277
What we test for:
Lactobacilli
Common BV related bacteria
Candida
Mycoplasma hominis
Ureaplasma
Gonorrhea
Chlamydia
Trichomoniasis
Mycoplasma genitalium
HPV16
HPV18
12 other high-risk HPV types
Microbiome + STI Screen
£188
What we test for:
Chlamydia
Gonorrhea
Trichomoniasis
Mycoplasma genitalium
Lactobacilli
Common BV related bacteria
Candida
Mycoplasma hominis
Ureaplasma
Microbiome Screen
What we test for:
Lactobacilli
Common BV related bacteria
Candida
Mycoplasma hominis
Mycoplasma genitalium
Ureaplasma

Wait, the vaginal micro-what?
Like your gut, your vagina is home to billions of bacteria (some good, some bad). These make up your vaginal microbiome. When it doesn’t contain enough good bacteria, you’re at greater risk of vaginal dryness, fertility challenges, as well as infections like STIs, thrush and BV.
Which pathogens do we test for?
With cutting-edge PCR technology for unparalleled accuracy, Daye tampons collect more vaginal fluid than a standard swab and cover the whole vaginal canal.
Lactobacilli
Good bacteria in your vaginal microbiome.
Anaerobic bacteria
Cause infections like bacterial vaginosis (BV).
Candida
Candida is a fungus which affects 75% of women.
Mycoplasma/ Ureaplasma
According to studies, can affect fertility.
Chlamydia
A very common STI caused by a bacterial infection.
*Only available with the STI Screen
Gonorrhoea
An STI that can affect both men and women.
*Only available with the STI Screen
Trichomoniasis
One of the most common STIs worldwide.
*Only available with the STI Screen
HPV screening
Detects the presence of high risk human papillomavirus strains.
*Only available with the HPV Screen
Herpes Type I & II
Can potentially infect another person.
*Only available with the STI Screen
What is included with every screening?
Order your test & get a kit delivered to your door
The kit will arrive at your doorstep in a discreet package. No more awkward queuing in clinic waiting rooms.

Collect and send off your sample to our accredited lab
Activate your kit with your unique code, complete a short symptom questionnaire, and send your sample - we'll handle the rest.

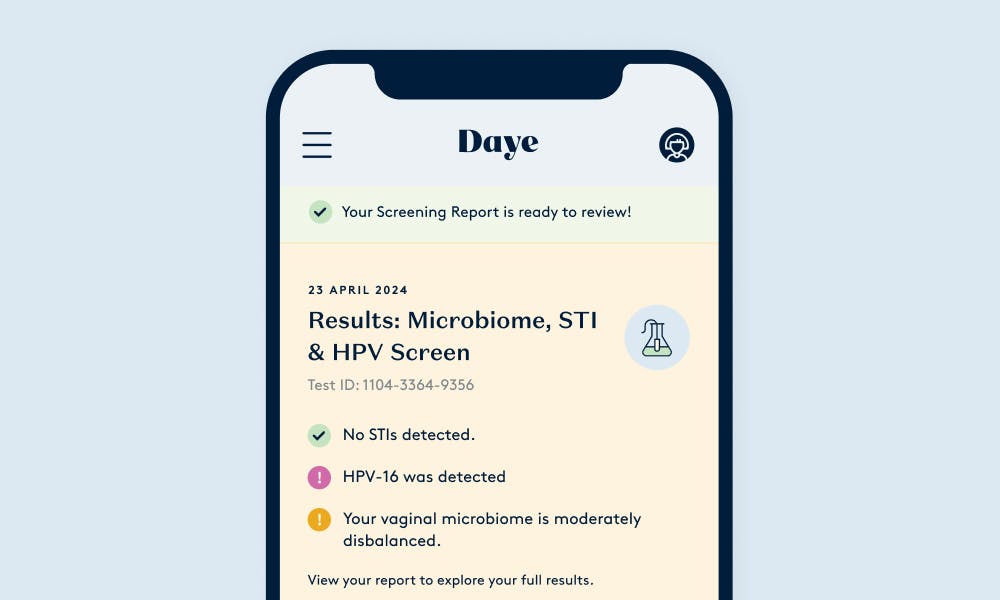
Get detailed, actionable results.
We never want to leave you stuck with a set of confusing or potentially troubling results. If you test positive for an STI, one of our sexual health nurses will provide a free consultation.
Connect with vetted specialists & get prescription treatments to your doorstep.
After the screening, you can set up virtual consultations with our vetted sexual health, fertility, and menopause experts. You can also get treatments discreetly delivered to your door.

Discover simple changes you can implement to take control of your health
Every report includes science-backed, personalised insights into lifestyle changes you can adopt to further enhance your health.

Be your own health hero
Got an infection that keeps coming back?
Got an infection that keeps coming back?
Mainstream treatments for BV and thrush can put us at a higher risk of recurrent infections.
Learn moreOwn your fertility journey.
Own your fertility journey.
A healthy microbiome is vital for successful fertilisation, implantation, and embryo development.
Learn moreWorried about STIs?
Worried about STIs?
As many as 70% of female STIs are asymptomatic, making proactive screening essential.
Learn moreSee our Founder’s results!
Wondering what we test for, and what results look like? Enter your email below and Valentina, our Founder, will send you her screening report.
By entering your email above you agree to receive marketing emails and promotions from Daye.


Your data is for your eyes only
Protecting your privacy is the least we can do
Frequently asked questions
Still have questions? Read all of our FAQs.
Think of it as the immune system to your reproductive tract. It contains good bacteria (lactobacilli) and disruptive microorganisms (yeasts, viruses). A healthy vaginal microbiome is one where the good bacteria keep the disruptive ones in check, preventing them from growing out of control and causing an infection. A balanced microbiome has been linked to a lower risk of vaginal infections, STIs, and reproductive difficulties. Understanding your vaginal microbiome composition can help you better manage your gynaecological health.
The tampon offers a non-invasive, familiar method of obtaining a testing sample that makes the screening experience at home more comfortable and accessible. Further, tampons collect a comprehensive sample from the entirety of the vaginal canal, allowing for greater accuracy compared to traditional methods like swabs. The applicator enables smooth insertion in the vagina, and it also prevents the tampon from being contaminated during insertion.
There are several studies that show the correlation between having a healthy vaginal microbiome and a lower risk of getting vaginal infections like thrush and BV, a lower risk of contracting STIs, improved fertility and lower risks of miscarriage and pre-term birth, and a lower risk of developing gynaecological cancers. You can find more study references at the bottom of the vaginal microbiome screening page, as well as in your test results.
You should always speak with your physician before committing to purchasing a diagnostic test. However, not all physicians are experts in the vaginal microbiome or have time to keep on top of the latest research (for example, did you know that Bacterial Vaginosis was only recognised as an STI in 2021?)
The Daye screen uses novel, PCR-based technologies, and the interpretation of our data are informed by modern clinical studies, which can give you additional, richer insights into what's happening with your gynaecological health. Keep in mind it can take a while (usually 10-15 years) for new research to be put into medical practice, so don’t be surprised if your doctor hasn’t heard of the vaginal microbiome yet.
Don’t let that stop you from taking charge of your health, especially if you’re experiencing recurrent infections or trying to conceive. Recent studies (we have linked some of them at the bottom of this page) have shown just how important the microbiome is for vaginal, sexual, and reproductive health.
We will analyse your microbiome for lactobacilli (the good, protective bacteria), Gardnerella vaginalis and Prevotella (anaerobic bacteria, linked to bacterial vaginosis), Candida (a yeast linked to thrush), Mycoplasma hominis, Mycoplasma genitalium and Ureaplasma parvum and urealyticum, commonly linked to reproductive difficulties and vaginal infections.
When you use the Daye Diagnostic Tampon, your sample is analysed in accredited clinical laboratories, and the results you receive will cover high-risk HPV strains, common STIs ( Chlamydia, Trichomoniasis and Gonorrhoea), and vaginal infections like Bacterial Vaginosis, Thrush, Ureaplasma and Mycoplasma.
Our reports tell you exactly which pathogens were detected, using validated qPCR assays and ISO-accredited laboratory processes.
These results meet clinical standards and can be used directly for treatment, referral, or follow-up with your GP, sexual health clinic, or gynaecologist.
If your results show something that needs attention, we’ll explain what it means and guide you through the next steps so you can access the right care quickly.After your sample reaches our lab, it will be analysed within 5–10 days. You will receive an email notification when your results are ready for review, or if there was an issue with your sample.
After you receive your results, you will be able to book a consultation with a vetted specialist and order medication (subject to additional costs and availability). We also help you make lifestyle changes to improve your gynaecological health. Did you know that everything from your contraception and condoms to underwear materials, can impact the composition of good and bad bacteria in your vagina? Stay in the know with Daye's screen and invest in interventions that actually work.
Our test uses quantitative PCR technology, which is able to quantify the relative amounts of microorganisms in your microbiome. While most GP/GU clinics use a method called microscopy to evaluate samples for pathogens causing BV or thrush, this requires a skilled technician to identify the presence of specific bacteria and differentiate them from one another. Microscopy is hence more subjective than DNA-based methods (like PCR) which detect the DNA of all microorganisms found in the sample in an automated way. Studies have shown that PCR is a more accurate way of assessing the bacterial composition of the vaginal canal than microscopy.
In practice, the PCR-based Daye screening results can point out if Gardnerella vaginalis (a common cause of BV) makes up 1% or 40% of a microbiome. Their amount is important because even though these bacteria are commonly found in a healthy microbiome, they can cause inflammation if they grow excessively.
We use certified labs in both the UK and US to test samples and process your results. Our UK partner labs are UKAS and CQC certified, while our US labs are CLIA and CAP certified. We also use CE-marked PCR panels. These certifications ensure our testing meets high quality standards.
In order to take a sample at least 5 days must have passed since your last period ended. There are a few other requirements: no antibiotics or antifungals in the last 30 days, no douching, penetrative vaginal sex, and vaginally applied meds or creams in the 24 hours before. That will ensure your microbiome is in a stable state and that your results are not inconclusive.
Using the kit at home is super easy — you just need to insert the provided tampon, wear it for at least 20 minutes (and up to 8 hours), and then put it in the pouches you have received in the kit, and ship it back to us in the same box you received initially. We’ve prepared detailed video instructions which you’ll see after completing the test activation questionnaire in your account.
- 2 tampons to take your sample — one to take your sample with and one for backup (double check the expiry date)
- A blue sterile pouch to keep the tampon sample safe from contamination
- A see-through shock-proof pouch to ensure the sample is protected on its way to the lab
- A 10 ml container with a transport medium liquid to protect your sample while on its way to the lab
- Step-by-step instructions on how to do the test + a card with the activation code
- For your convenience, the return label, which you can use to ship your sample back to our partner lab, is already attached to the outside of the box.
Don’t use the kit if any of these is missing or damaged. Get in touch with our customer care team and we’ll sort it out.
At Daye, we believe in building products that are rooted in scientific rigour. This means that we never want to get ahead of the science available. Like many other areas of gynaecological health, vaginal microbiome research has been underfunded for decades.
Vaginal microbiome screening is also not a common practice in clinical care today unless you go private.
A vaginal microbiome screen is used to understand the composition of bacteria in your vaginal microbiome. This can help you identify the presence of pathogens, which could be causing you recurrent vaginal infections (Candida, Gardnerella) or preventing you from becoming pregnant (Ureaplasma, Mycoplasma). If you're peri-menopausal or menopausal, you may want to increase your lactobacilli count so as to fight off vaginal dryness. If you have suffered recurrent UTIs, you may find a disrupted vaginal microbiome to be the cause. Knowing that you have a low lactobacilli count can also help you and your physician make informed decisions on your risk of a recurrent miscarriage or pre-term labour.
Not every physician, however, will recommend a vaginal microbiome screen, due to the method not being widespread yet. Please feel free to consult with your doctor before purchasing this test. If you require a simple bacterial vaginosis or candida test, you can get one for free from your local sexual health clinic.
It's also important to note that by testing your vaginal microbiome you are contributing to an increased global understanding of the best ways to detect and manage gynaecological health diseases, in turn bridging the gender gap in medical research and innovation.
Tampons can potentially stretch or tear the hymen, but it's not a guaranteed or common occurrence. The hymen is a thin membrane that partially covers the opening of the vagina in some individuals. It can vary in thickness and elasticity from person to person. When inserting a tampon, if done carefully and gently, it typically shouldn't cause damage to the hymen. However, if a person's hymen is particularly thin or if they have a medical condition called imperforate hymen (where the hymen completely covers the vaginal opening), there is a slightly higher chance of the tampon causing some stretching or tearing.
It's important to note that the hymen can naturally stretch or tear over time due to various activities such as physical activity, horseback riding, gymnastics, or even normal vaginal development. Sexual activity can also impact the hymen, but it's not the only factor in hymen integrity. In many cultures, there is a misconception that an intact hymen is a sign of virginity, but this is not a reliable indicator. Hymens can vary greatly in appearance and resilience, and not all individuals with intact hymens have never engaged in sexual activity.We recommend avoiding the use of the tampon for vaginal diagnostics for a period of six weeks following vaginal birth. This allows ample time for the body to heal and reduces the risk of potential complications. Please consult with your healthcare provider for guidance specific to your individual situation.
In addition to the postpartum period, we advise against using the tampon for vaginal diagnostics if you have any open wounds, sores, or other vaginal irritations. It is essential to prioritize your comfort and well-being, and if you have any concerns, please consult your healthcare provider.
If you experience any discomfort, unusual symptoms, or adverse reactions while using the tampon for vaginal diagnostics, we recommend removing it immediately and consulting with your healthcare provider. Your health and safety are our utmost priority, and it is essential to address any concerns promptly.
Our Vaginal Microbiome Screening specifically detects the relative abundance of Lactobacilli and Anaerobic bacteria as a percentage of all bacteria in the sample. Very high levels of Lactobacilli (>80% of all bacteria) are generally associated with a healthy microbiome. Increased levels of anaerobic bacteria, such as Gardnerella, Porphyromonas and Prevotella spp. may suggest a higher risk of bacterial vaginosis (BV). While our screening offers valuable information, it is essential to remember that these results are not diagnostic on their own. To gain a comprehensive understanding of your vaginal health, it's important to discuss your results alongside your medical history and any symptoms you may be experiencing with a healthcare professional. Once you receive your screening report from Daye, you will be able connect with vetted specialists online.
While our nurses and vetted specialists can provide valuable insights and guidance, they can't formally diagnose conditions through Daye's platform. Our service is designed to help detect potential issues, but it's not a substitute for an in-person medical diagnosis.
However, we do offer a convenient pharmacy service. We partner with licensed prescribing pharmacists who can review your medical history and screening results. If appropriate, they can provide prescriptions for certain conditions like bacterial vaginosis or thrush, which can then be delivered discreetly to your door. This service offers a convenient way to access treatment for common gynaecological issues. For more complex concerns or if you're unsure, we still recommend following up with a healthcare provider for a comprehensive evaluation. Remember, your health and wellbeing are our top priority, and we're here to empower you with knowledge, resources, and convenient care options when possible.
Our diagnostic tampon screening service is only available to people aged 18 and over. This age requirement is in place due to regulatory reasons and because our service is designed for adults who can legally consent to medical screening and handling of sensitive health data without parental permission. The 18+ requirement ensures we're operating within legal and ethical guidelines for healthcare services.
If you're under 18, we recommend visiting your GP or a local sexual health clinic where appropriate services for young people are available. Many sexual health clinics offer free and confidential services specifically designed for teenagers.
Relevant Research
Diagnosis of bacterial vaginosis on self-collected vaginal tampon specimens
2002 • P D J Sturm, P Moodley, G Nzimande
Results of the tampon and vaginal smears showed excellent agreement for both observers (Spearman >0.80). The overall sensitivity and specificity were 91.7% (95% CI: 81.6-96.5) and 79.3% (95% CI: 67.2-87.8), respectively, using the Amsel criteria as reference standard. The tampon provides a specimen for the combined diagnosis of non-ulcerative STIs and BV.
A Self-Administered Technique for the Detection of Sexually Transmitted Diseases in Remote Communities
1997 • Sepehr N. Tabrizi, Barbara Paterson, Christopher K. Fairley, Francis J. Bowden, Suzanne M. Garland
The detection of each organism was significantly greater by PCR in tampon-collected samples than by routine conventional methods (P < .01).
Pilot study of the utility and acceptability of tampon sampling for the diagnosis of Neisseria gonorrhoeae and Chlamydia trachomatis infections by duplex realtime polymerase chain reaction in United Kingdom sex workers
2010 • P T Kimmitt, S N Tabrizi, M Crosatti, S M Garland Frcpa, P C Schober, K Rajakumar, C A Chapman
Besides near-universal acceptability of tampon sampling, the tampon sampling–PCR approach described in this study appeared to have enhanced sensitivity compared with conventional testing.
Vaginal microbiome and sexually transmitted infections: an epidemiologic perspective
2011 • Rebecca M. Brotman
Vaginal bacterial communities are thought to help prevent sexually transmitted infections. Bacterial vaginosis (BV) is a common clinical syndrome in which the protective lactic acid-producing bacteria (mainly species of the Lactobacillus genus) are supplanted by a diverse array of anaerobic bacteria. Epidemiologically, BV has been shown to be an independent risk factor for adverse outcomes including pre-term birth, development of pelvic inflammatory disease, and acquisition of sexually transmitted infections. Longitudinal studies of the vaginal microbiome using molecular techniques such as 16S ribosomal DNA analysis may lead to interventions that shift the vaginal microbiota toward more protective states.
The Vaginal Microenvironment: The Physiologic Role of Lactobacilli
2018 • Emmanuel Amabebe, Dilly O. C. Anumba
Lactobacilli and their antimicrobial and anti-inflammatory products along with components of the epithelial mucosal barrier provide an effective first-line defence against invading pathogens including bacterial vaginosis, aerobic vaginitis-associated bacteria, viruses, fungi and protozoa. An optimal host-microbial interaction is required for the maintenance of eubiosis and vaginal health.
The role of Escherichia coli in reproductive health
2017 • P Cools
Vaginal dysbiosis has been associated with increased susceptibility to and transmission of HIV and other sexually transmitted infections and increased risk of pelvic inflammatory disease, pre-term birth and maternal and neonatal infections.
Pregnancy's Stronghold on the Vaginal Microbiome
2014 • Marina R. S. Walther-António, Patricio Jeraldo, Margret E. Berg Miller, Carl J. Yeoman, Karen E. Nelson, Brenda A. Wilson, Bryan A. White, Nicholas Chia, Douglas J. Creedon
Our analyses indicate normal pregnancy is characterised by a microbiome that has low diversity and high stability. While Lactobacillus species strongly dominate the vaginal environment during pregnancy across the two studied ethnicities, observed differences between the longitudinal dynamics of the analysed populations may contribute to divergent risk for pregnancy complications. This helps establish a baseline for investigating the role of the microbiome in complications of pregnancy such as pre-term labour and pre-term delivery.
The vaginal microbiome as a tool to predict IVF success
2020 • Sam Schoenmakers, Joop Laven
The vaginal composition prior to the start of hormonal treatment for ART seems to be predictive of in vitro fertilization/in vitro fertilization-intracytoplasmic sperm injection (IVF/IVF-ICSI) outcome, with mainly a highly negative predictive value.
Early pregnancy vaginal microbiome trends and pre-term birth
2017 • Molly J. Stout, Yanjiao Zhou, Kristine M. Wylie, Phillip I. Tarr, George A. Macones, Methodius G. Tuuli
In a predominantly African-American population, a significant decrease of vaginal microbial community richness and diversity is associated with pre-term birth. The timing of this suppression appears early in pregnancy, between the first and second trimesters, suggesting that early gestation may be an ecologically important time for events that ordain subsequent term and pre-term birth outcomes.
The role of the vaginal microbiome in gynaecological cancer
2017 • M Champer, A M Wong, J Champer, I L Brito, P W Messer, J Y Hou, J D Wright
Human microbiome research has shown commensal bacteria to be a major factor in both wellness and disease pathogenesis. Interest in the microbiome has recently expanded beyond the gut to include a multitude of other organ systems for which the microbiome may have health implications. Here, we review the role of the vaginal microbiome in health and disease, with a particular focus on gynecologic malignancies. Further, we suggest that it may be possible to expand the use of probiotics in the treatment of gynaecological cancers.
Association between polycystic ovary syndrome and the vaginal microbiome: A case-control study
2020 • Xiang Hong, Pengfei Qin, Kaiping Huang, Xiaoling Ding, Jun Ma, Yan Xuan, Xiaoyue Zhu, Danhong Peng, Bei Wang
There was significant difference in vaginal bacterial structures between PCOS and healthy control women. The relative abundance of Lactobacillus crispatus in the PCOS group was significantly lower than controls (P = .001), and the relative abundance of Mycoplasma and Prevotella was higher than controls (P < .001, P = .002, respectively). The Mycoplasma genus could be a potential biomarker for PCOS screening, as ROC analysis showed that the area under the curve (AUC) for the relative abundance of Mycoplasma was 0.958 (95% CI: 0.901-0.999).
Menstrual Tampons Are Reliable and Acceptable Tools to Self-Collect Vaginal Microbiome Samples
2023 • Florence Turner, Josephine Drury, Dharani K Hapangama, Nicola Tempest
Many women report embarrassment as the cause for their avoidance of routine gynaecological screening appointments. Methods of self-collection of bio samples would perhaps encourage women to participate in routine screening programs. The vaginal microbiome plays a key role in women's health and reproductive function. Microbial disturbances can result in the loss of lactobacillus dominance, also known as dysbiosis, associated with an increased risk of contracting sexually transmitted infections (STIs), pregnancy complications and infertility. All (100%) of volunteers were happy to provide a tampon as a sample for testing. The findings from this study show that tampons and LVSs were comparable when analysing the vaginal microbiome, with potential superiority of the tampon with regard to patient acceptability.














